When two drugs are taken together, they don’t just sit side by side in your body. They interact-sometimes in ways that save lives, and sometimes in ways that land you in the hospital. Most people know that one drug can affect how another is absorbed or broken down. But far fewer understand what happens when drugs meet at their target sites. This is where pharmacodynamic drug interactions come in. Unlike pharmacokinetic interactions (which change how much drug is in your blood), pharmacodynamic interactions change how the drug works-even when the concentration stays exactly the same.
How Pharmacodynamic Interactions Work
Think of your body’s receptors like locks. Drugs are keys. A pharmacodynamic interaction happens when one key changes how another key fits into the lock-or even blocks it entirely. The drug’s concentration doesn’t drop. It’s still there. But its effect? That’s altered. This is why two drugs with perfectly safe doses on their own can become dangerous when combined.
According to research from European teaching hospitals (2015-2017), about 40% of serious drug interactions in hospital settings are pharmacodynamic. These aren’t rare edge cases. They’re common enough that medical boards like the CICM require doctors to memorize specific examples. The three main types are:
- Additive: The combined effect equals the sum of each drug alone. Like taking two painkillers that both reduce inflammation-your pain relief doubles.
- Synergistic: The combined effect is stronger than the sum. This is the good kind-when doctors intentionally pair drugs to get more bang for the buck.
- Antagonistic: One drug cancels out or reduces the effect of the other. This is the dangerous kind-especially when it’s unintentional.
Receptor Competition: When Drugs Fight for the Same Spot
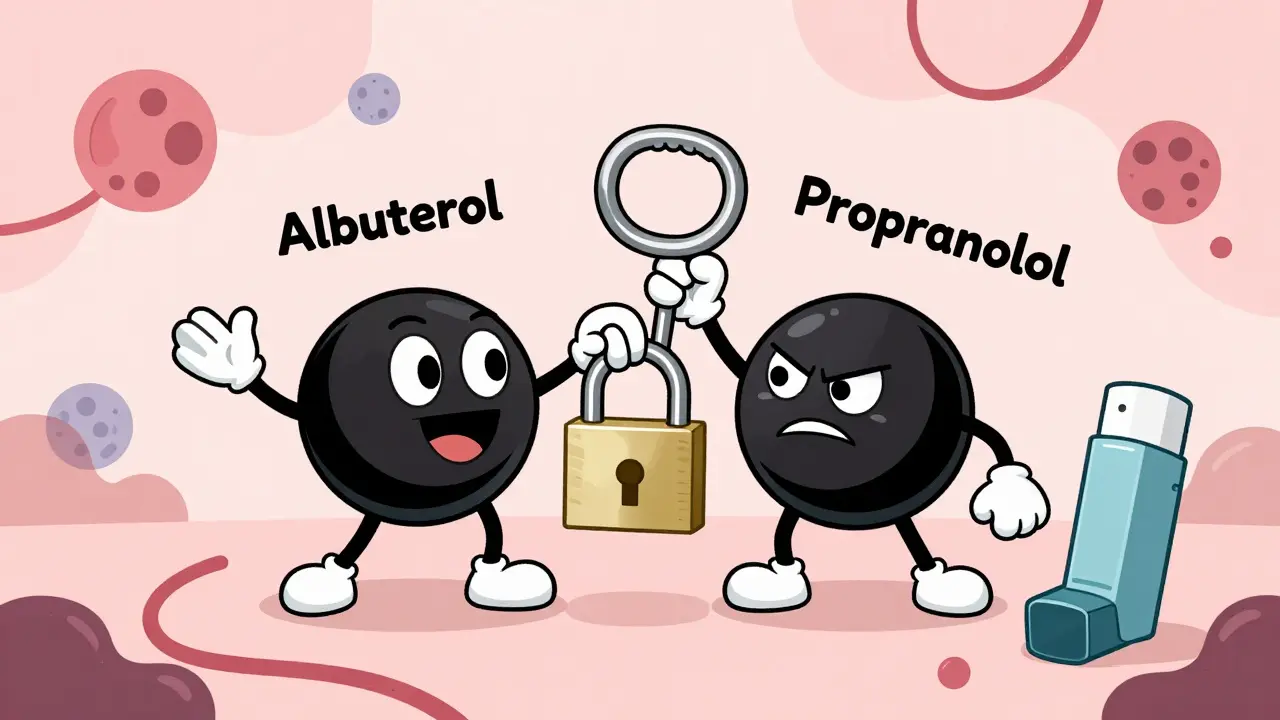
One of the most straightforward mechanisms is receptor competition. Two drugs bind to the same receptor, and the one with higher affinity wins. Take albuterol and propranolol. Albuterol opens up airways by activating beta-2 receptors. Propranolol blocks those same receptors to lower heart rate. If you take both, propranolol can completely block albuterol’s effect. For someone with asthma, that’s not just inconvenient-it’s life-threatening.
Merck Manual’s 2023 data shows that drugs with higher receptor affinity (measured in nanomolar concentrations) dominate these battles. A patient on beta-blockers for high blood pressure who suddenly needs an inhaler for a flare-up might not realize their rescue medication just became useless. This isn’t theoretical. It’s documented in emergency rooms across the UK and US.
Physiological Interference: When Drugs Work Against Each Other’s System
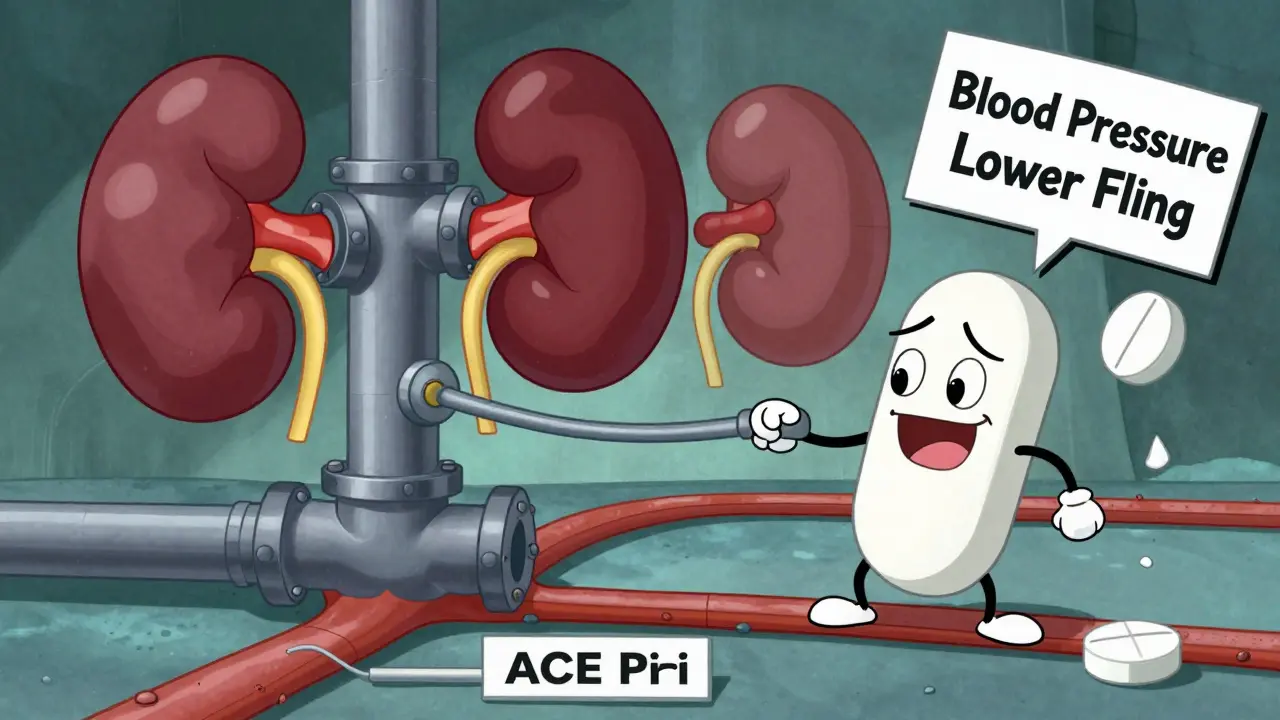
Not all interactions happen at the same receptor. Sometimes, drugs mess with the body’s own systems. A classic example is NSAIDs like ibuprofen and ACE inhibitors like lisinopril. ACE inhibitors lower blood pressure by relaxing blood vessels. Ibuprofen reduces inflammation by blocking prostaglandins-chemicals that help keep kidney blood flow steady. When you take both, ibuprofen cuts renal blood flow by about 25%, making the ACE inhibitor far less effective. A 2019 NIH study of 347 hypertensive patients showed this combo led to uncontrolled blood pressure in nearly 40% of cases.
This is why doctors often warn patients on blood pressure meds to avoid over-the-counter painkillers. It’s not about liver damage-it’s about the drug losing its power. And patients rarely connect the dots. They take Advil for a headache, don’t feel any difference in their BP, and assume the medicine isn’t working. In reality, the interaction is silently undermining treatment.
Antagonism Gone Wrong: The Most Dangerous Combinations
Some pharmacodynamic interactions are so dangerous they’re outright contraindicated. The NHS Specialist Pharmacy Service lists 287 such interactions as “potentially harmful and contraindicated.” Among the worst:
- SSRIs + MAOIs: Combining antidepressants like sertraline with MAOIs like phenelzine can trigger serotonin syndrome-a potentially fatal condition with fever, seizures, and muscle rigidity. A 2021 meta-analysis found this combo increases serotonin syndrome risk by 24-fold.
- Opioids + Opioid Antagonists: Giving naloxone to someone dependent on morphine doesn’t just reverse the pain relief-it triggers full-blown withdrawal. In a hospital, this can cause cardiac arrest. In a hospice setting, it can turn comfort care into trauma.
- Anticoagulants + Antiplatelets: Warfarin and aspirin together increase bleeding risk far beyond what either drug does alone. A 2022 survey of 1,247 physicians found this was the most common dangerous interaction, accounting for 38% of monthly cases.
One Reddit user-a hospital pharmacist-shared a near-fatal case: a 78-year-old on linezolid (an antibiotic) and sertraline developed serotonin syndrome. She spent 72 hours in intensive care. The interaction wasn’t flagged by the hospital’s EHR system. The pharmacist caught it only because she recognized the drug names from her own study notes.
The Hidden Gold: When Interactions Save Lives
Not all pharmacodynamic interactions are bad. In fact, some of the most powerful drugs in medicine rely on them. Trimethoprim and sulfamethoxazole (Bactrim) are a perfect example. Each drug blocks a different step in bacterial folic acid production. Together, they shut down the pathway completely. A 2018 study showed this combo reduced the needed dose of each drug by 75% compared to using either alone-making it more effective and less toxic.
Even more surprising: low-dose naltrexone (an opioid blocker) combined with antidepressants has shown promise in treatment-resistant depression. A 2021 study in the Journal of the American Pharmacists Association found that 68% of patients improved with the combo, compared to 42% on antidepressants alone. The theory? Low-dose naltrexone may tweak immune signaling in the brain, making antidepressants work better. This isn’t theory-it’s clinical data.

Why This Matters More Than Ever
People are taking more drugs than ever. The average person over 65 takes 4.8 prescription medications. By 2050, there will be 1.5 billion people over 65 worldwide. More drugs = more chances for hidden interactions. The FDA now requires pharmacodynamic interaction studies for all new CNS drugs. The European Medicines Agency reports 34% of new drug applications include this data-up from 19% in 2015.
But technology isn’t catching up fast enough. A 2020 study in Drug Safety found clinical decision systems miss 22% of serious pharmacodynamic interactions. Why? Because they’re built on simple rules: “Don’t mix A and B.” They don’t understand receptor affinity, physiological pathways, or dose-response curves.
The most effective solution? Pharmacist-led reviews. A 2021 BMJ Quality & Safety review found pharmacist interventions reduced adverse events by 58% in elderly patients. In 92% of those cases, the prevented interaction involved NSAIDs and antihypertensives.
What You Can Do
- Know your drugs: If you’re on more than three medications, ask your pharmacist: “Could any of these cancel each other out?”
- Watch for sudden changes: If your blood pressure suddenly spikes, or your asthma inhaler stops working, ask if a new drug might be interfering.
- Check for narrow therapeutic index drugs: These are drugs where the difference between a dose that works and one that kills is tiny. Examples: warfarin, digoxin, lithium, theophylline. Any interaction with these can be deadly.
- Don’t assume OTC is safe: Ibuprofen, naproxen, even some herbal supplements (like St. John’s Wort) can trigger dangerous interactions.
Pharmacodynamic interactions aren’t about bad doctors or careless patients. They’re about complexity. The human body doesn’t handle drugs like a simple list. It handles them like a symphony-where one wrong note can ruin the whole piece. Understanding these interactions isn’t just for pharmacologists. It’s for anyone taking more than one pill a day.
What’s the difference between pharmacodynamic and pharmacokinetic drug interactions?
Pharmacokinetic interactions change how your body processes a drug-like how fast it’s absorbed, broken down, or cleared. For example, grapefruit juice can block a liver enzyme that breaks down statins, making the drug build up to toxic levels. Pharmacodynamic interactions don’t change drug levels. Instead, they change how the drug works at its target. One drug might block a receptor, alter a physiological response, or boost another drug’s effect-without changing its concentration in your blood.
Can over-the-counter drugs cause pharmacodynamic interactions?
Absolutely. Common OTC painkillers like ibuprofen and naproxen can reduce the effectiveness of blood pressure medications by interfering with kidney function. Even antacids with magnesium or aluminum can alter how your body responds to certain antibiotics. St. John’s Wort, a popular herbal supplement, can reduce the effect of birth control pills and antidepressants by altering serotonin pathways. Just because it’s sold without a prescription doesn’t mean it’s safe to mix.
Why do some drug interactions only show up after months of use?
Some interactions build slowly. For example, long-term NSAID use with an ACE inhibitor gradually reduces kidney perfusion. The effect isn’t immediate-it takes weeks for blood flow to drop enough to impact drug effectiveness. Similarly, the body may adapt to one drug over time, making the second drug’s interference more noticeable later. That’s why a patient might take two drugs for months without issue, then suddenly develop high blood pressure or worsening asthma.
Are pharmacodynamic interactions more dangerous than pharmacokinetic ones?
In terms of severity, yes. A 2020 analysis of FDA data found that 68% of serious adverse events from pharmacodynamic interactions led to hospitalization, compared to 42% for pharmacokinetic ones. Why? Because pharmacodynamic interactions often affect critical systems like heart rhythm, breathing, or brain chemistry. When two drugs clash at the receptor level, the result can be sudden and catastrophic-like serotonin syndrome or withdrawal from opioid antagonists. Pharmacokinetic interactions, while dangerous, usually develop more slowly and can often be managed with dose adjustments.
How can I find out if my medications interact?
Start by asking your pharmacist. They have access to databases like the NHS Specialist Pharmacy Service’s drug interaction tool, which tracks over 1,800 pharmacodynamic interactions. Online tools like the University of Liverpool’s HIV Drug Interactions database are reliable for specific drug classes. But no app or website replaces a human review. If you’re on five or more medications, request a full medication review from your pharmacist-it’s free on the NHS and often covered by insurance elsewhere.
 Mar, 22 2026
Mar, 22 2026
Jacob Hessler
March 22, 2026 AT 23:49Danielle Arnold
March 24, 2026 AT 09:41Brandon Shatley
March 25, 2026 AT 03:48Natasha Rodríguez Lara
March 26, 2026 AT 15:21James Moreau
March 27, 2026 AT 16:15Blessing Ogboso
March 29, 2026 AT 14:29Kenneth Jones
March 30, 2026 AT 12:08Mihir Patel
March 30, 2026 AT 18:55Caroline Bonner
March 31, 2026 AT 06:22peter vencken
March 31, 2026 AT 15:48Chris Crosson
March 31, 2026 AT 20:11Linda Foster
April 1, 2026 AT 05:48Darlene Gomez
April 3, 2026 AT 03:23Katie Putbrese
April 4, 2026 AT 20:36